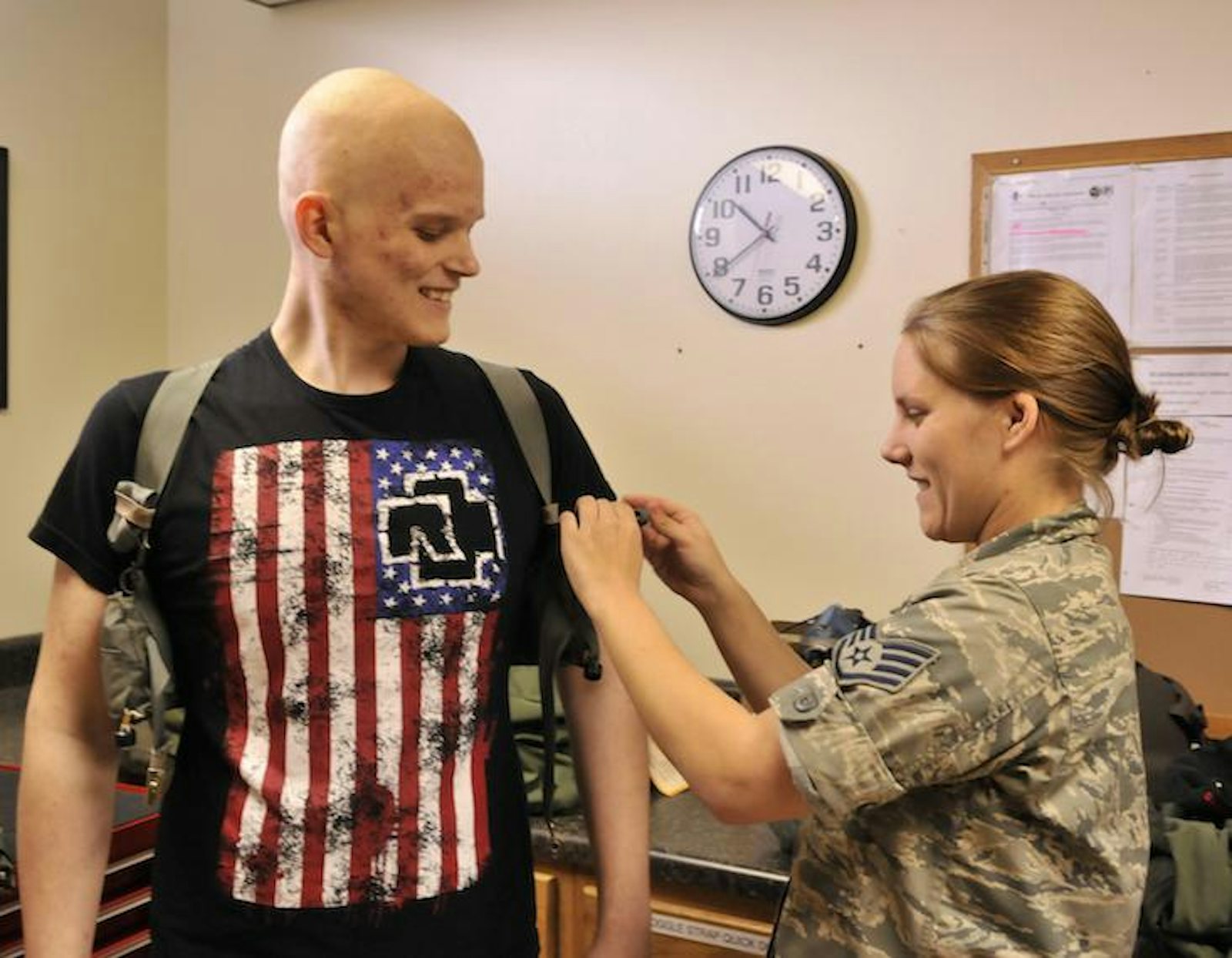
I treated an inspiring teenage girl in my clinic the other day. Although Sadie has made a complete recovery from her liver cancer and bears no physical scars from the treatment, anxiety and depression followed her through childhood and adolescence. Last year, I introduced her to our local support group for these adolescent young-adults patients, 13thirty Cancer Connect, and she’s blossomed. She hangs out at their local center weekly, has countless new friends, all of whom had or have cancer, and goes on field trips and other programs with them. Her comfort in her own skin and her smile spoke to a young girl transformed. When I commented on this, she said, “I finally found a group of friends who get it.”
For a while, oncologists didn’t. Many were, both during and after these young patients’ treatment, often oblivious to and ill-equipped to meet their needs. They didn’t appreciate that few young cancer patients—after being diagnosed with cancer and undergoing treatment for a few months or years—pick up life where it left off. Instead, physical and cognitive or emotional scars remain for many of them, and that shouldn’t be surprising: For young people, appearance and finding peer groups—at school or in sports or in other ways—can be vital. Loneliness, depression, and the fear of recurrence can prolong these patients’ dependence on parents, preventing them from living full lives. So the vast majority emerge from their disease changed people and struggle to find, what they term, “a new normal.”
Oncologists are beginning to “get it” now. A 2012 paper highlighted the unique “psychosocial challenges” adolescent-young-adult cancer patients face. And a study from March of this year found that these patients “have significantly worse social functioning scores around the time of diagnosis, at the 12-month follow-up, and at the 24-month follow-up when compared with population norms.” The National Cancer Institute (NCI) has called on medical institutions in the U.S. to design programs to help meet these needs, provides a great deal of invaluable information to adolescents and young adults, funds research in this area, and offers clinical support for oncologists and patients. There is even an academic journal, The Journal of Adolescent and Young Adult Oncology, which explores all aspects of cancer in adolescent-young adult patients.
There has also been an explosion of support groups online for adolescents and young adults themselves, which isn’t so surprising, given how internet-savvy they are.
All this speaks to the growing recognition of the unique needs of adolescents and young adults with cancer, and how those needs differ from younger children and older adults. Many teens, young adults, and their families knew this long before we did, and have contributed to improving medical and psychosocial care for teens and young adults through their strong, even heroic advocacy. Take Lauren Spiker, for example. In 2002, she founded 13thirty Cancer Connect, the group to whom I had referred Sadie. Originally named Melissa’s Living Legacy Foundation, Spiker was inspired to create this group by her daughter, Melissa, who died of leukemia at age 19.1 Spiker realized, far sooner and far more than most of us oncologists did, that cancer uniquely disrupts and threatens teens and young adults’ lives. Hers was one of the first organizations dedicated to these young people. With a strong in-person and online presence, 13Thirty Cancer Connect has blossomed into a remarkable organization that has helped fill an important void in the care of teens and young adults with cancer.
Adolescent-young adult (AYA) cancer patients range in age from 15 to 39, as somewhat arbitrarily defined by the NCI. The NCI has taken an active role in highlighting the unique needs of the AYA group, bringing together interested subspecialists and conducting several workshops focusing on the basics of this population: What diseases do they get? What are their unique challenges? How can we best help them?
A proportionate amount of resources dedicated to their care might be a good start. Approximately 70,000 young people in this age range are diagnosed with cancer every year in the U.S, yet the less-than 10,000 children under 15 diagnosed with cancer annually in the U.S. have considerably more resources available to help them. What’s more, the types of cancers this group gets are different than what pediatric oncologists see in their younger patients and what adult oncologists see in their older patients. (Some of the more commonly seen types of cancer include leukemia, lymphoma, melanoma, tumors of bones and muscles and ligaments, tumors of the reproductive system, thyroid cancers and spinal cord tumors.)
Cleaning up the referral patterns between pediatric and adult oncologists would help as well. It is rather messy; there is no standard. It varies from community to community, from hospital to hospital, and even within a given hospital: A 19-year-old with leukemia might be seen by a pediatric oncology group in Rochester, New York, but in New York City by an adult oncology group. You might think that shouldn’t really matter—aren’t both groups well trained to treat patients with leukemia? Yes, but the pediatric group, accustomed to administering high dose intensive therapy to a generally younger population, might be prone to treat more intensively than a 19-year-old can handle; adult oncologists, on the other hand, might be cautious in their approach, their experience tempered by the side effects their decades-older patients suffer.
Solving this issue, among others, will require these oncologists to work together. One might think that shouldn’t be that difficult; after all, they are all oncologists! However, the two groups grow up in two very different medical cultures (pediatrics vs adult medicine), are trained in different ways, see patients with different diseases, and often practice in separate places. So the challenges of creating a jointly administered adolescent-young adult oncology program are considerable.
We can be thankful for those emboldened by the challenge. A wonderful organization started, in England, by Roger Daltrey and Pete Townshend of the venerable rock group, the Who, has dedicated itself to confronting these obstacles. Its mission is “to partner with hospitals throughout the United States to develop specialized facilities and services for teens and young adults with cancer.” There has also been an explosion of support groups online for adolescents and young adults themselves, which isn’t so surprising, given how internet-savvy they are. The NCI website lists some of these groups, including one with a national presence, Stupid Cancer (formerly known as I’m too Young for this, or I2Y), as well as the organization inspired by Melissa, 13Thirty Cancer Connect; as helpful as online support is, though, nothing matches face-to-face, peer-to-peer connections.
Somehow, in some way, I have to believe that Melissa, who left this earth 17 years ago, was listening and smiling and thinking, “Cool! Hey Mom, we have made a difference!”
David Korones is a pediatric hematologist/oncologist and palliative care physician at the University of Rochester Medical Center in Rochester, New York.
1. With her last words, Melissa, Spiker’s daughter, asked her mother to help people like her, teens and young adults with cancer. “Do something, Mom,” she said. “Do something that will make some sense of this; that will make a difference so that kids don’t have to travel down the same road I did.”
WATCH: The meaning of “personalized medicine all the way down.”
This article was originally published on Cancer Focus in December 2017.