
Last July, Chris Perry went on an Alaskan cruise with her family to celebrate her parents’ 50th wedding anniversary. When she boarded the massive Norwegian Sun cruise ship, she felt “a little woozy and weird” from the boat’s gentle rocking, she remembers, but the sensation quickly faded. Perry didn’t feel seasick at all during the rest of the cruise, and spent a happy week marveling at the glaciers. But while standing in the Anchorage airport to catch her flight home to San Francisco, she suddenly felt the ground moving under her, undulating with the gentle rhythm of waves.
Many people have experienced this sensation after getting off a boat; they may sway or stagger until their vestibular system re-adapts to stationary ground and they get their “land legs” back. For most people, the feeling vanishes within minutes or hours. But in rare cases, and for mysterious reasons, the illusion persists for months or even years. Perry is one of those unlucky ones, a sufferer from the disorder rather poetically dubbed Mal de Debarquement syndrome.
Perry has felt the world bobbing beneath her feet for nearly four months now. She also had the constant sensation that her body was swaying in a clockwise circular motion, as if she were balancing on an unsteady deck. These feelings never stopped, and they completely disrupted her life. Over the months, she discovered which activities made her disorientation worse: looking down (chopping vegetables and doing dishes became problematic), focusing on something close-up (ditto for reading), sitting still with her eyes closed (so much for meditating), and being under bright fluorescent lights (forget about grocery shopping).
Perry grappled not just with daily discomfort, but also with the fear that something in her brain was permanently broken. “I cry every day,” she recently told me. She had seen a succession of doctors, neurologists, and inner-ear specialists, but none of them could help. Physical therapy didn’t do any good, and a prescription for Klonopin, a Valium-like drug that both reduces anxiety and suppresses the action of the vestibular system, only reduced her symptoms for short stretches.
“They’re going to put me in a magic spinning room,” she said wryly. “I hope so much they can fix me.”
But there’s new hope for Perry and for others, like her, who are internally out to sea. Their salvation may be found in a small, windowless lab at Mount Sinai Hospital in New York City. Here neurologist Mingjia Dai thinks he has discovered not only the faulty mechanism behind Mal de Debarquement syndrome (the name is French for “disembarkation sickness”), but also the first therapy that treats it effectively. So Perry, feeling desperate, flew to New York last week and paid $1,000 for the experimental treatment. “They’re going to put me in a magic spinning room,” she said wryly. “I hope so much they can fix me.”
Dai’s method involves fixing the vestibulo-ocular reflex, the neural mechanism that stabilizes images on the retina when the head is in motion. This reflex causes the eyes to move in the opposite direction of the head’s motion, a compensation tactic that allows a person to maintain focus on an object while her body is moving. (The vestibulo-ocular reflex is tamped down in people who spin much more than normal, like figure skaters, one of the many ways the brain contributes to athletic performance.) Dai’s research suggests that, in people like Perry, the reflex adapted too well to the motion of the boat, and needs to be readapted to life on land. In July he published positive results showing that the treatment cured or substantially helped 70% of subjects. Since then he has received a stream of patients from all over the country.
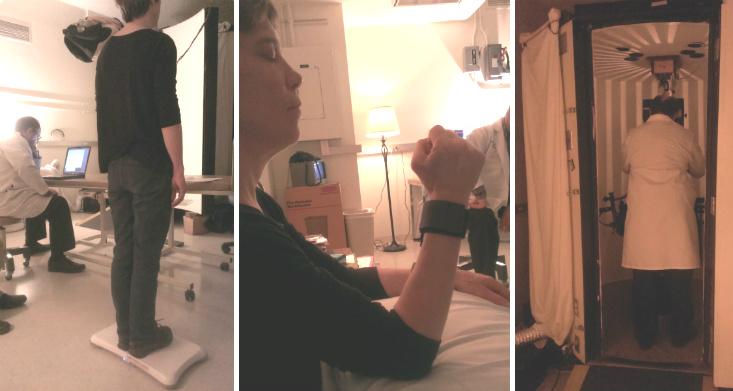
On Monday, during Perry’s first treatment session, Dai set out to measure her perceived motions. Perry stood on a Wii Balance Board that contains pressure sensors; on a connected computer, Dai and a colleague watched Perry’s center of balance shift in a slow, clockwise circle. Next the doctors told Perry to sit down, strapped an accelerometer to her wrist, and asked her to move her arm in time with her perceived circular swaying motions. Both of these tests revealed the same frequency of motion: Perry’s internal deck was completing its rocking motion once every seven seconds.
Finally Perry was ready for treatment. Dai told her to enter the chamber, a small octagonal room about six feet wide, and sit down. Dai’s colleague, Sergei Yakushin, programmed a sequencer to play an ascending musical scale in seven seconds, and then go back down in another seven seconds. Yakushin took hold of Perry’s head and began rocking it from side to side in time with the scale. Then Dai turned on the projector inside the chamber, and vertical black and white stripes began revolving slowly around the walls and ceiling, encompassing Perry’s entire field of vision. The stripes and the tinny musical notes reminded Perry of “a carnival sideshow,” she said later.
The idea behind Dai’s treatment is to create a visual experience that re-trains the vestibulo-ocular reflex. As Perry took in a striped world moving constantly to the right, her reflex compensated by moving her eyes to the left. This equal and opposite reaction, Dai posited, would cancel out the unnecessary compensation that Perry’s brain had been constantly performing—the clockwise circular swaying she has perceived for four months straight.
When Perry emerged from the chamber on Monday, she stood with her eyes closed for a few moments and focused on her sensations. “I feel the circular motion less,” she reported. But she still felt the floor bobbing beneath her. So Dai timed the frequency of the bobbing, then sent her back into the chamber to watch horizontal stripes move down the walls.
Monday’s session was just the beginning; Perry went to Mount Sinai all week for treatments. By Wednesday her sensation of bodily motion was almost completely gone, and the Wii Balance Board confirmed that she was no longer swaying in circles. “That was the part that was really agitating,” she said, “I do feel better, for sure.” However, Dai’s treatment didn’t succeed in taking away her perception of the ground surging beneath her feet. The doctor told her to take heart, Perry says, and said that sensation too will likely fade away in the coming months, particularly if she stays off the Klonopin medication that was suppressing the activity of her vestibular system and preventing it from readjusting. Perry says that after four destabilizing months, she’s finally feeling hopeful. “I’m halfway off the boat,” she says.
Eliza Strickland is an associate editor for the science and technology magazine IEEE Spectrum.


























