Mangroves are sturdy trees. Recognizable by their extensive root systems, these trees can thrive in muddy soil, sand, peat, even coral. They tolerate water much saltier than most other plants and survive flooding during severe storms. It is perhaps their sturdiness that led mangroves to be one of the most significant targets in the Vietnam War.
During the war, communist guerilla fighters would often take refuge in Vietnam’s thick jungles. Mangroves, among other types of flora, provided shelter from eyes in the sky seeking to deliver air strikes in strategic locations. So the U.S. military exposed guerillas by bombarding the trees themselves with huge amounts of defoliants, chemical herbicides that cause the leaves to fall off of plants. The most infamous defoliant was Agent Orange, named for the orange stripes marking the drums it was shipped in.
The defoliant is an equal mix of two herbicides, 2,4-diclorophenoxyacetic acide (2,4-D) and 2,4,5-trichlorophenoxyacetic acid (2,4,5-T). When sprayed on foliage during the war, it quickly stripped off the leaves, revealing anyone and anything below the canopy, destroying crops, and clearing vegetation near U.S. bases. By the end of the campaign, U.S. military forces had sprayed millions of gallons of Agent Orange on over 5 million acres of upland and mangrove forests and about 500,000 acres of crops—an area the size of Massachusetts, and about 24 percent of South Vietnam. Some areas of Laos and Cambodia along the Vietnam border were also sprayed. This massive effort, known as Operation Ranch Hand, lasted from 1962 to 1971.

Unfortunately, the story doesn’t end there. Although the main goal of Operation Ranch Hand was aimed at destroying trees rather than killing or causing harm to humans, the impacts of Agent Orange on both environmental and human health are manifold, and the scientific community has yet to develop a robust understanding of them.
To start with what we do know, the herbicides by themselves prove toxic to foliage and are associated with risks to human health in high doses. Furthermore, the 2,4,5-T in Agent Orange was contaminated by dioxins, a family of chemicals that form during manufacturing processes and can be extremely toxic to humans. The primary and most toxic dioxin in Agent Orange is 2,3,7,8-tetrachlorodibenzo-p-dioxin, better known as TCDD.
People who live in areas that were heavily exposed to Agent Orange can end up consuming small but biologically significant amounts of dioxin through the food chain. The other major route of exposure is through direct skin absorption, which was more common when Agent Orange was being sprayed in the 1970s.
“Oil and water don’t mix,” explains Peter Kahn, Professor of Biochemistry at Rutgers School of Environmental and Biological Sciences, who has devoted much of his research on the effects of Agent Orange exposure to U.S. Vietnam veterans. “Dioxin is oil soluble, and oil is a hydrocarbon. Anything that is soluble in one hydrocarbon is soluble in others.” That means that dioxins are just as soluble in cooking oils as they are in adipose tissue or other fats in the human body.
Once in the body, dioxin stays there awhile. The half-life of dioxin in the body is seven years, meaning that after that long, the concentration will fall to half its original level. If you’ve done your math, you may have noticed that also means someone who had a large exposure to dioxin during the war would have nearly rid it from their body by now. However, lingering dioxin traces in the environment can still find their way into people’s bodies, either from contact with or through food grown in contaminated soil.

Kahn began his research on Agent Orange as a postgraduate student in New York City. Enraged by the use of chemical warfare by the U.S. military, he recognized a gap in research and went on to become one of a few scholars dedicated to understanding Agent Orange’s effects on human health. His collaborative work with another dioxin chemist in Sweden, Christoffer Rappe, eventually led to a 13-year stint on a New Jersey State commission researching Agent Orange’s effects on U.S. veterans. Kahn’s research is part of a body of work that has found dioxin poisoning linked to soft-tissue sarcoma and non-Hodgkin lymphoma (two forms of cancer), various physiological birth defects like spina bifida, skin rashes, among other varied health problems.
In Vietnamese, illnesses related to Agent Orange are sometimes called da cam or, “orange skin,” for the lesions that appear after exposure to high doses.
Medical treatment comes in the form of pain relief—anything from modern pain medicine to traditional medicine to holistic approaches like massage. There is no cure. Just triage.
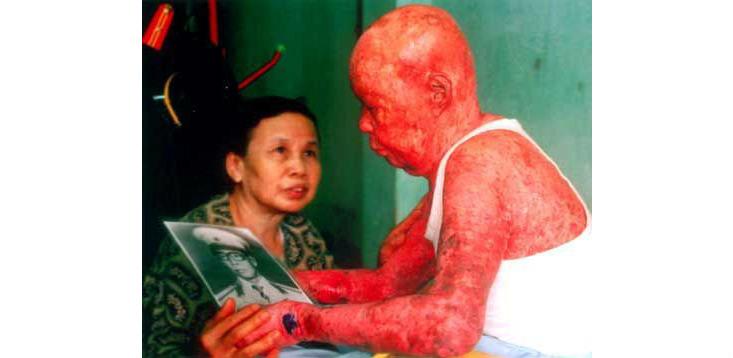
Pinning down the extent of this chemical plague is difficult. As current research stands, scientists have a good understanding of what happens in “sudden, single-issue exposure” to dioxin, such as in industrial accidents. For example, exposure in high doses can lead to skin ailments like chloracne, which looks like adolescent acne but can be severe and persist throughout one’s lifetime. High doses can also increase risk of digestive problems, cancers, and birth defects.
However, trying to figure out the health effects of chronic exposure to low doses is more difficult. The main reason is that effects of dioxin are not always immediate. They can be delayed a decade or two, even longer. Effects can also be subtle. Even so, the Red Cross estimates that close to three million Vietnamese people have been affected by Agent Orange since the war, including 150,000 children.
Getting a better handle on the effects of Agent Orange and the prevalence of those effects could potentially take decades. In comparison, our understanding of tobacco’s effects on human health is based on decades-long studies of enormous populations starting in the 1950s. “Vietnam’s entire population would make up only a fraction of the number of people involved in medical studies about tobacco,” Kahn offers, for perspective.
Though much needed, care is not available to many people suffering from dioxin exposure. Many patients can’t afford to stay in hospitals or “peace villages,” special organizations that have formed in Vietnam and other affected areas to provide care for patients suffering from Agent Orange-related ailments.
Foreign aid from the U.S. toward alleviating the effects of Agent Orange has been focused on environmental remediation rather than health care. In 2010, the U.S. announced a $44 million initiative called the Đà Nẵng Airport Remediation Project to remove dioxin residue around the former U.S. airbase in Đà Nẵng, one of the identified “hot spots” for dioxin contamination. The highest level recorded in a person was 1,000 parts per trillion, found in someone fishing in the lake on the Đà Nẵng airbase, compared to a baseline of around 2–7 parts per trillion for people living in nations that haven’t been heavily exposed.
The the need for aid to alleviate patients’ suffering is paramount and, in some ways, is more immediate than the need for research to find out how dioxins affect us. Under these circumstances, it may do more damage to wait for science to catch up to what is happening to Agent Orange patients. Dr. Kahn suggests,“If you have sick people, take care of them. Worry about the science afterwards. If it takes 40 years, so be it.”
Special thanks to Dr. Peter Kahn, Dr. Mai Thanh Truyết, Peter and Mary Lidgard, and Pham Ngoc Mai.
Lily Bui is a graduate researcher in MIT’s Comparative Media Studies program. She is the daughter of two Vietnamese immigrants. Tweets @dangerbui.
Further information:
Vietnamese Association of Victims of Agent Orange (VAVA)
Vietnam: My Orange Pain, RTD Films (2014)
The Last Ghost of War (2008)
“The Vietnam Syndrome,” Vanity Fair
Make Agent Orange History
Agent Orange and Cancer
Public Health Virginia: Agent Orange conditions




























